HPV vaccine as cancer prevention is a message that needs to catch on
New infection stats should be ‘a wake-up call’ to spur lagging vaccination rates
SURE SHOT In the United States, HPV vaccination rates lag for girls and boys. The message that the vaccine prevents cancer isn’t getting out there, researchers say.
Judy Schmidt/CDC
Cancer prevention isn’t the first thing that comes to many parents’ minds when they consider vaccinating their preteens against human papillomavirus, or HPV. And the fact that HPV is transmitted sexually gives the vaccine more baggage than a crowded international flight. But what gets lost in the din is the goal of vaccination, to protect adolescents from infection with HPV types that are responsible for numerous cancers.
Newly released estimates show just how prevalent HPV infections are in the United States. In April, the U.S. Centers for Disease Control and Prevention reported for 2013-2014 that among adults ages 18 to 59, 25 percent of men and 20 percent of women had genital infections with HPV types that put them at risk of developing cancer.
That’s just a snapshot in time. For those who are sexually active, more than 90 percent of men and 80 percent of women can expect to become infected with at least one type of HPV during their lives. About half of those infections will be with a high-risk HPV type.
“People who think, ‘I’m not at risk,’ are really not understanding the magnitude of this virus,” says cancer epidemiologist Electra Paskett of Ohio State University in Columbus.
HPV is the most common sexually transmitted infection in the United States. The HPV group of viruses includes low-risk and high-risk types. Low-risk types 6 and 11 are responsible for 90 percent of all genital warts. The high-risk types of HPV can cause cancer, and the two behind most HPV-related cancers are types 16 and 18. Seventy percent of cervical cancers can be traced back to types 16 and 18, while type 16 also causes cancers of the anus, vagina, penis and the oropharynx, the part of the throat at the back of the mouth. HPV spreads by sexual contact, either vaginal, anal or oral.
Story continues below graph
Short of the finish
In 2015, only four in 10 girls and three in 10 boys were fully vaccinated against HPV, according to estimates from the U.S. Centers for Disease Control and Prevention. This falls well short of the national goal of eight in 10 adolescents.
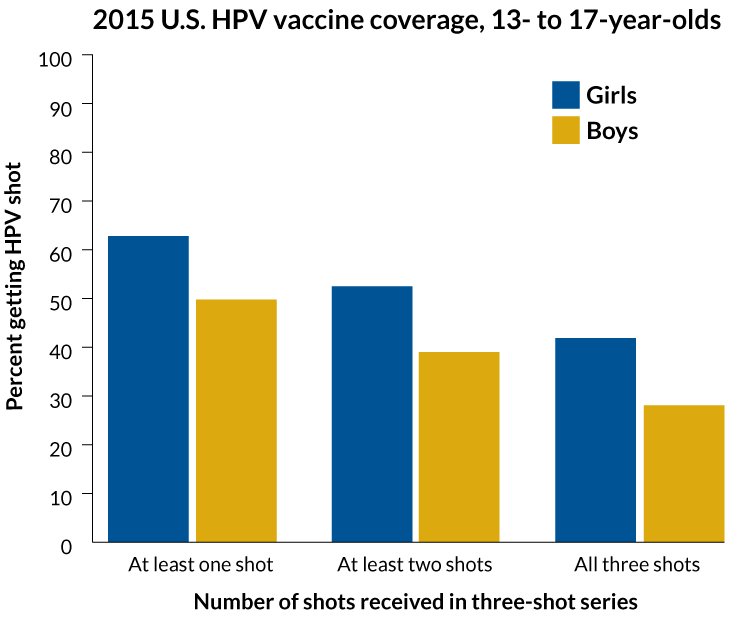
Source: CDC
Nationally, from 2011 to 2014, 11 percent of men ages 18 to 69 had an oral infection with any type of HPV, and for nearly 7 percent of men, it was a high-risk type, the CDC’s National Center for Health Statistics estimated in its April report. For women in this age group, it was 3 percent and 1 percent, respectively.
The numbers are far worse when it comes to genital HPV infections. During 2013 to 2014, 45 percent of men and 40 percent of women ages 18 to 59 had genital infections with any type of HPV. One in four men and one in five women in this age group were infected with a high-risk type.
“It’s a wake-up call for both genders, but particularly for males,” says Jessica Keim-Malpass, a nurse scientist at the University of Virginia in Charlottesville.
For an estimated 19,200 women and 11,600 men each year, HPV infections result in a cancer diagnosis.
Vaccination could greatly relieve this cancer burden. Three different HPV vaccines have been available in the United States. The first, introduced in 2006, covered low-risk types 6 and 11 and high-risk types 16 and 18. The most recent HPV vaccine protects against these four types as well as five more high-risk types, and is the only vaccine currently distributed nationally. A federal advisory committee recommended routine vaccination against HPV at 11 or 12 years of age in 2006 for girls and in 2011 for boys.
But the HPV-cancer prevention message doesn’t seem to be getting through in the United States. HPV vaccination rates lag behind the national coverage goal of 80 percent for 13- to 15-year-olds. In 2015, among U.S. adolescents ages 13 to 17, six out of 10 girls and five out of 10 boys had gotten at least one shot in a three-shot series. But only four out of 10 girls and three out of 10 boys had completed the series.
What’s with the lackluster response?
Parents are part of the issue. “They don’t know about the vaccine, or they have fears about safety, or they say ‘My child is not going to be at risk for HPV infections,’” Paskett says.
The safety of all three vaccines was established in large clinical trials before approval by the U.S. Food and Drug Administration. Since 2006, almost 90 million doses of HPV vaccines have been administered nationally, and the most common side effects are soreness or swelling at the site of the shot.
Some parents think that “by giving the vaccine, you are saying it’s OK to have sex,” notes Keim-Malpass. Research doesn’t back this up. A 2012 study in Pediatrics of 11- to 12-year-old girls found that HPV vaccination was not tied to increased sexual activity, as measured by medical records of sexually-transmitted infection or pregnancy. A 2015 study in JAMA Internal Medicine of 12- to 18-year-old girls found no evidence to link HPV vaccination with higher rates of sexually transmitted infections.
The recommended age for vaccination ensures that preteens are protected before they are exposed to HPV, whenever that may be. “The whole reason the vaccine is targeted to 11- and 12-year-olds is to get kids vaccinated before they enter a sexual relationship,” says Keim-Malpass.
Lack of urgency is a problem, too. The delay between an infection and a future cancer can make people complacent about HPV. “You are protecting yourself from an infection, but it has ramifications years, decades later,” Keim-Malpass says. “It’s not about something you get tomorrow, it’s about something you could get 20 to 30 years from now.”
Another difficulty has been the vaccination schedule. The initial recommendation was for three doses, with the second shot one to two months after the first, and the third shot six months after the first. This schedule was challenging for busy adolescents, notes Keim-Malpass.
Now there is a new dosing regimen. For adolescents who begin vaccination before turning 15, only two shots are required, with the second one coming six to 12 months after the first. This should be easier to accommodate in yearly well-child visits.
Even with the suboptimal vaccination rates, there has been an impact on infections. A 2016 Pediatrics study found that, within six years of the first vaccine’s introduction in 2006, infections with the four HPV types covered decreased 64 percent among 14- to 19-year-old girls. There are also fewer cases of genital warts among U.S. teens since 2006.
Any decline in infection rates is a good thing. But “it’s not to the extent we could have, if from the get- go, people realized this was a cancer vaccine,” says Paskett. “If there was a vaccine for breast cancer, moms would be lining up around the corner with their daughters.”







