Widely used antidepressants may reduce the ominous brain plaques associated with Alzheimer’s disease, a new study in mice and humans finds.
Brain scans of people who have taken antidepressants reveal fewer clumps of the protein amyloid-beta, a target of Alzheimer’s prevention strategies, when compared with people who have not taken the drugs.
Many in the field voiced caution about the results. But if borne out by further study, the findings may point to a new, relatively safe way to treat and prevent Alzheimer’s disease, which is the sixth leading cause of death in the United States.
“I think this is a wonderful piece of news, and I think there’s going to be a lot of excitement about this,” says internist Michael Weiner, who leads the Alzheimer’s Disease Neuroimaging Initiative at the Veterans Affairs Medical Center campus of the University of California, San Francisco. “It points the way towards a possible approach to treating Alzheimer’s disease that people have not been talking about very much.”
In the study, mice genetically engineered to overproduce amyloid-beta, or A-beta, were given one of three selective serotonin reuptake inhibitors, a class of antidepressants that boost circulating levels of the chemical messenger serotonin in the brain. After a single dose of the antidepressants, A-beta levels dropped in the fluid that surrounds mouse brain cells, researchers report online the week of August 22 in the Proceedings of the National Academy of Sciences. A full day after receiving the drug, the mice’s A-beta levels fell by nearly a quarter.
Long-term, chronic administration of the drug had a larger effect. Engineered mice that took the SSRI citalopram for four months had about half the A-beta plaques in their brains as mice that hadn’t had the drug. This reduction seems to happen through a protein called ERK, which serves as the middleman between brain cells’ serotonin-sensing proteins and A-beta production.
Figuring out the details of this process may open the door for developing new ways to prevent A-beta buildup, says study coauthor John Cirrito of the Washington University School of Medicine in St. Louis.
To see if a similar effect might be happening in people, the scientists scanned the brains of 186 cognitively normal elderly people and looked for signs of A-beta plaques. The team used a compound called PIB that binds to big clumps of A-beta in the brain and glows on a PET scan.
Of these participants, 52 reported that they had taken an antidepressant in the last five years. These people, researchers found, had about half the A-beta load in their brains as the people who hadn’t taken an antidepressant. What’s more, the length of time the participants took the drugs correlated with the density of A-beta plaques in the brain — the longer the antidepressant dose, the less plaque.
“We think there are influences going in two opposite directions,” says study coauthor and psychiatrist Yvette Sheline, also of Washington University. “We think depression pushes you toward dementia, but antidepressant treatment pushes you toward protection.”
Finding similar results in mice and humans lends the study credibility, Weiner says. “When you have animal data and human data coming together, then you start to get really excited,” he says.
Still, Weiner and others caution that it would be premature to conclude that antidepressants protect against A-beta buildup or that fewer plaques necessarily translate into less disease.
The study uncovered an association — not a clear-cut cause and effect, Weiner notes. “We cannot say with certainty that the reason why people who took the SSRIs have lower cortical amyloid is due to the fact that they took SSRIs,” he says.
And molecular neuroscientist Heather Snyder of the Alzheimer’s Association in Chicago points out that even if antidepressants are shown to reduce A-beta, scientists still don’t know how A-beta levels affect the brain. “We don’t really know what modulating amyloid will do to cognition,” she says. “And we don’t know if we need to reduce it by 10 percent or 20 percent, or if it needs to be completely reversed.”
Another confounding factor is that A-beta can take several forms in the brain, from small molecules to large, sticky clumps, and some forms may be more dangerous than others. Interpreting the A-beta clumps that PIB detects in human brain scans remains challenging.
“We’re being very cautious,” Cirrito says. “There are a lot of people on these drugs and we don’t want to get anybody overly excited without reason.” He and his colleagues plan to test whether acute doses of SSRIs change A-beta levels in the cerebrospinal fluid of healthy human subjects.
Even if the new findings are replicated in larger studies, a major question about Alzheimer’s and antidepressants remains, Sheline says. “The real question is — which this paper sheds no light on — does that mean that long-term, they [SSRI-treated people] will have less of a risk of dementia? And that’s exactly the big study that needs to be done.”
Back Story | Alzheimer’s on the rise
Though the link between Alzheimer’s and depression is murky, both diseases are major public health concerns. Among people 65 and older, one in eight has Alzheimer’s disease; an estimated one of 11 adults overall report depression. Current drugs can effectively combat depression in most cases, but nothing exists to prevent Alzheimer’s. Right now, Alzheimer’s is the fifth leading cause of death in people 65 years and older. And unlike other major diseases such as heart disease and stroke, which caused fewer deaths in 2008 than in 2000, Alzheimer’s deaths rose by 66 percent in that time (see graph). With the oldest of the baby boomers turning 65 this year, that trend is expected to worsen.
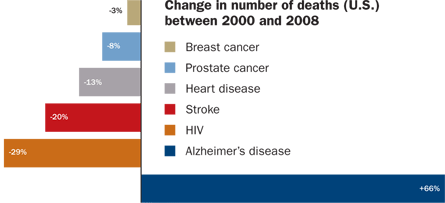 Source: Alzheimer’s Association
Source: Alzheimer’s Association







