CRISPR gene editing moved into new territory in 2017
Debates about when and how to use the tool in humans take on new urgency
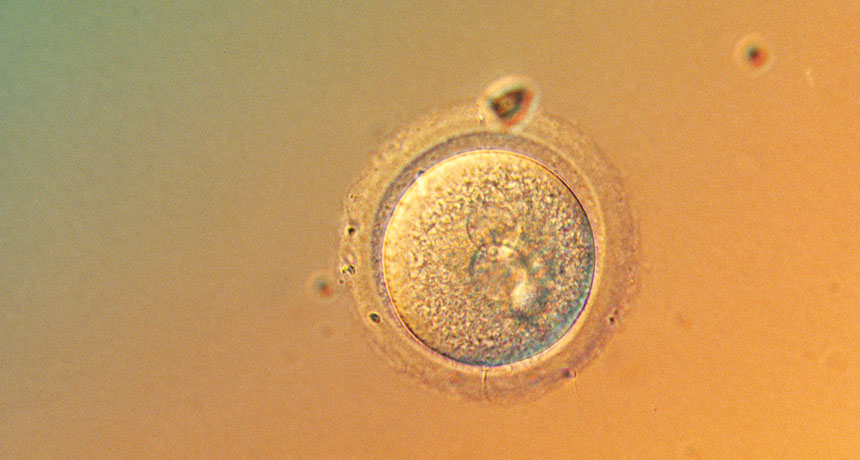
HUMAN DEBUT In the last year, research teams have announced CRISPR gene editing in viable human embryos (single-cell embryo shown).
Claude Cortier/Science Source