ENVIRONMENTAL EXPOSURES Things people come in contact with every day, such as pesticides, chemicals in water, hormone-mimicking chemicals in cash register receipts, smoke and air pollution, can change chemical tags on DNA and proteins. What those changes mean and how useful they are for determining health risks aren’t yet clear.
Clockwise from top left: Ittipon/Shutterstock; Gyvafoto/Shutterstock; BILLION PHOTOS/SHUTTERSTOCK; ZURIJETA/SHUTTERSTOCK
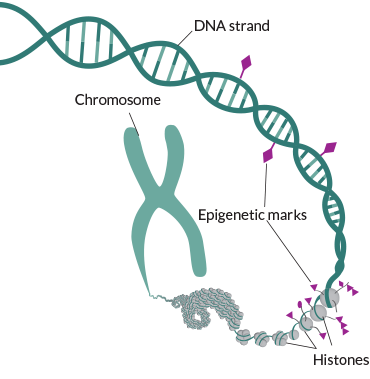
Nearly everything people do, eat or come into contact with can change them in little ways — sometimes with big consequences. Exposure to some chemicals can damage DNA, leading to cancer and other problems. Other molecular changes—chemical tags added to DNA or to proteins called histones — may affect health without injuring DNA.
There are more than 100 varieties of these chemical tags, collectively known as epigenetic marks. While they may help humans and other organisms respond to their environments, the tags can also alter development and body functions in unhelpful, even harmful, ways. Yet people who make decisions about safe levels of exposure to chemicals, heavy metals and other environmental factors generally aren’t including epigenetic alterations in their deliberations.
Risk assessors take a wide variety of scientific data into account when making recommendations for preventing overexposure to chemicals. When it comes to epigenetic information, though, “honestly, we don’t know what to do with it,” says Marie Fortin, a toxicologist and risk assessor for Colgate-Palmolive Co. “We don’t have a framework to interpret it,” she said at the Society of Toxicology’s ToxicoEpigenetics meeting in Tysons Corner, Va., in November.
Even researchers studying how environmental factors write, erase and tweak epigenetic marks admit that the field is in its infancy and still has a long way to go before it can be used to make public health decisions. Epigenetics is “a science that offers enormous opportunities for research, and maybe in a long time it will be useful for risk assessment, but right now we don’t know enough,” says neurotoxicologist Deborah Cory-Slechta of Rochester University Medical Center in New York.
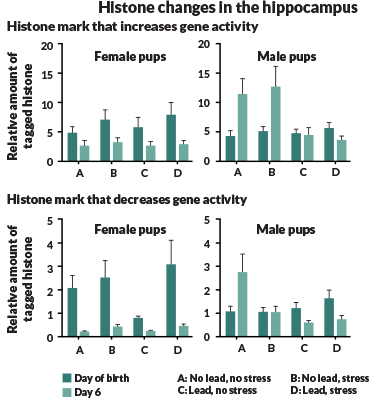
Cory-Slechta coauthored a paper describing the epigenetic effects of lead and stress on developing mouse brains. Studying those changes may help scientists learn how lead impairs human brain function and may suggest ways to counteract the heavy metal’s effects, she says.
Stressed mouse moms that drank water laced with lead during pregnancy had offspring in which two important epigenetic marks differed in parts of their brains, Cory-Slechta and colleagues reported in the May NeuroToxicology. At various times during development, male and female pups had different changes in the hippocampus, a brain structure involved in learning and memory. Those findings could indicate that males are at higher risk of developing learning problems when their mothers are exposed to lead and are under stress.
Other epigenetic studies have indicated that high-fat diets, smoking, exposure to pesticides or to estrogen-mimicking chemicals could have health effects — including increased risk of breast and other cancers—that last for generations (SN: 4/6/13, p. 18). A study published in Scientific Reports in 2015 indicated that grandchildren could inherit epigenetic marks if their grandmothers were exposed to lead (SN: 3/19/16, p. 8). And researchers regularly publish new studies showing that epigenetic marks can be altered by exposure to air pollution, arsenic in drinking water or chemicals such as bisphenol A that are found in products including plastics, canned food and cash register receipts.
Yet there are limits to applying the conclusions to human risk assessment. For one thing, most of what scientists know about environmental effects on epigenetic marks comes from animal studies. Such studies will always be imperfect mimics of what goes on in humans.
One obstacle to using lab animals as stand-ins for humans is that the animals aren’t living in the real world. Researchers give lead to mice for only a short time, for example; humans typically face long-term exposures, Cory-Slechta says. Her mouse studies indicate that stress can make lead’s effects worse, but lab mice don’t deal with the same sort of social and economic stress that people do. Those types of chronic stress may have different epigenetic consequences than those produced by the short-lived physical challenges mice are usually subjected to.
Another major roadblock to determining whether mice and people respond similarly to lead exposure is that Cory-Slechta and her colleagues can’t get samples of people’s brains. The closest the researchers might get is examining epigenetic marks in people’s white blood cells, but lead is likely to affect those cells differently than it does brain cells.
Researchers also don’t agree on which epigenetic marks they should track. Some scientists favor DNA methylation, an alteration in which molecules called methyl groups are attached to the DNA building block cytosine. That mark usually signals that gene activity has been turned down.
Other researchers concentrate on chemical modifications of histones. Histones are proteins that form spools around which DNA is wound to fit into a cell. A dizzying array of chemical changes at various spots on the histones are associated with more or less gene activity. For instance, tacking an acetyl group onto the histone H3 protein at a specific spot is associated with increased gene activity, but switching the acetyl group for a couple of methyl groups can reduce gene activity. Researchers may not be able to get away with choosing just one of these epigenetic marks to predict how a chemical exposure, diet, exercise and stress might combine with a person’s age, sex and genetic makeup to affect them, says molecular toxicologist Shaun McCullough.
Each epigenetic mark is like a letter in a language, says McCullough, of the U.S. Environmental Protection Agency’s National Health and Environmental Effects Research Laboratory in Chapel Hill, N.C. If researchers look at only one type of modification, “it’s like trying to get something out of reading a book in which you can only see one of the letters. You’re not going to get the full story.”
Filling in all of the letters may not be necessary. Like contestants on Wheel of Fortune, researchers may be able to guess at the meaning of a particular epigenetic change with a few key letters. To play the guessing game, researchers may have to construct a database compiling all the epigenetic changes in response to particular chemicals and how these changes influence the activity of many genes. Such a project is still a dream; most researchers are still concentrating on only one mark at a time and its effect on a few genes.
Even if researchers learn to read the epigenetic language, they still need to establish whether changes cause disease, are merely indicators that something has gone wrong, or are neutral, says environmental epigeneticist Dana Dolinoy.
Dolinoy, of the University of Michigan School of Public Health in Ann Arbor, and McCullough co-organized the Toxico-Epigenetics meeting. Their goal was to bring policy makers and research scientists together to learn how epigenetics might be incorporated in risk assessment. Even though participants walked away from the conference with no definite answer, they have begun talking about the steps needed to determine whether epigenetic marks are reliable predictors of chemical exposure safety.
Regulators shouldn’t wait for epigenetics to mature as a field before making a ruling on safety, says Ivan Rusyn, a toxicologist at Texas A&M University in College Station. But they should keep the door open for revising decisions as more data become available.
Rusyn is one of 46 authors of a report in the November issue of Environmental Health Perspectives on the promise and challenges of incorporating new technology into risk assessment. He’s optimistic that epigenetics can one day contribute valuable data about health risks, but that day won’t come soon. “Right now this is not an airplane we can fly,” he says. “It’s an airplane that’s still in the drawing stage.”