How the new coronavirus stacks up against SARS and MERS
For the third time since around 2003, a coronavirus has jumped from animals to people
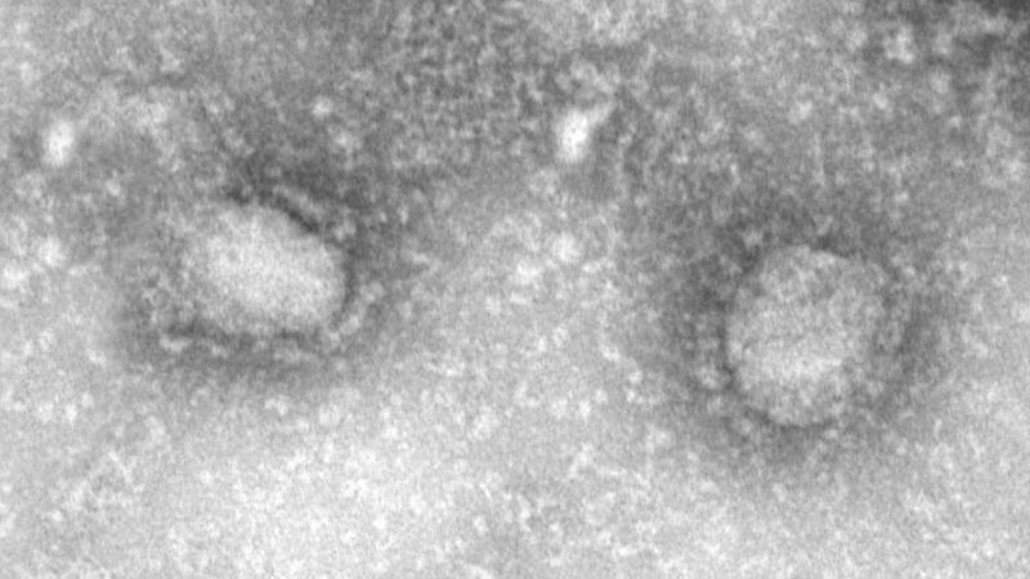
A new coronavirus called 2019 novel coronavirus, or 2019-nCoV, (seen here in a transmission electron micrograph) is spreading in China. It is similar to both SARS and MERS.
Courtesy: IVDC, China CDC via GISAID
- More than 2 years ago
Read another version of this article at Science News Explores
Coronaviruses, one of a variety of viruses that cause colds, have been making people cough and sneeze seemingly forever. But occasionally, a new version infects people and causes serious illness and deaths.
That is happening now with the coronavirus that has killed at least 26 people and sickened at least 900 since it emerged in central China in December. The World Health Organization is monitoring the virus’s spread to see whether it will turn into a global public health emergency (SN: 1/23/20).
Among the ill are two people in the United States who contracted the virus during travels in China. A Chicago woman in her 60s is the second U.S. case of the new coronavirus, the Centers for Disease Control and Prevention confirmed January 24 in a news conference.
Officials are currently monitoring 63 people across 22 states for signs of the pneumonia-like disease, including fever, cough and other respiratory symptoms. Of those people, 11 have tested negative for the virus. Two, including the newest case and another patient in Seattle, tested positive, the CDC reported (SN: 1/21/20).
France reported two cases on January 24 as well, the first in Europe.
Much still remains unknown about the new coronavirus (SN: 1/10/20), which for now is being called 2019 novel coronavirus, or 2019-nCoV. Lessons learned from previous coronavirus outbreaks, including severe acute respiratory syndrome, or SARS, and Middle East respiratory syndrome, or MERS, may help health officials head off some of the more serious consequences from this virus outbreak.
What are coronaviruses?
Coronaviruses are round and surrounded by a halo of spiky proteins, giving them a resemblance to a crown or the sun’s wispy corona.
Four major categories, or genera, of coronavirus exist. They’re known by the Greek letters alpha, beta, delta and gamma. Only alpha and beta coronaviruses are known to infect people. These viruses spread through the air, and just four types (known as 229E, NL63, OC43 and HKU1) are responsible for about 10 to 30 percent of colds around the world.
What makes a virus a coronavirus is only loosely enshrined in its DNA. “The coronavirus designation is less about the genetics and more about the way it appears under a microscope,” says Brent C. Satterfield, cofounder and chief scientific officer of Co-Diagnostics, a company based in Salt Lake City and Gujarat, India, that is developing molecular tests for diagnosing coronavirus infections.
Coronaviruses’ genetic makeup is composed of RNA, a single-stranded chemical cousin of DNA. Viruses in the family often aren’t very similar on the genetic level, with some types having more differences between them than humans have from elephants, Satterfield says.
The new virus’s proteins are between 70 and 99 percent identical to their counterparts in the SARS virus, says Karla Satchell, a microbiologist and immunologist at Northwestern University Feinberg School of Medicine in Chicago.

How dangerous is a coronavirus infection?
Usually coronavirus illnesses are fairly mild, affecting just the upper airway. But the new virus, as well as both SARS and MERS, are different.
Those three types of betacoronaviruses can latch onto proteins studding the outside of lung cells, and penetrate much deeper into the airway than cold-causing coronaviruses, says Anthony Fauci, director of the U.S. National Institute of Allergy and Infectious Diseases in Bethesda, M.D. The 2019 version is “a disease that causes more lung disease than sniffles,” Fauci says.
Damage to the lungs can make the viruses deadly. In 2003 and 2004, SARS killed nearly 10 percent of the 8,096 people in 29 countries who fell ill. A total of 774 people died, according to the World Health Organization.
MERS is even more deadly, claiming about 30 percent of people it infects. Unlike SARS, outbreaks of that virus are still simmering, Fauci says. Since 2012, MERS has caused 2,494 confirmed cases in 27 countries and killed 858 people.
MERS can spread from person to person, and some “superspreaders” have passed the virus on to many others. Most famously, 186 people contracted MERS after one businessman unwittingly brought the virus to South Korea in 2015 and spread it to others. Another superspreader who caught MERS from that man passed the virus to 82 people over just two days while being treated in a hospital emergency room (SN: 7/8/16).
Right now, 2019-nCoV appears to be less virulent, with about a 4 percent mortality rate. But that number is still a moving target as more cases are diagnosed, Fauci says. As of January 23, the new coronavirus had infected more than 581 people, with about a quarter of those becoming seriously ill, according to the WHO. By January 24, the number of reported infections had risen to at least 900.
An analysis of the illness in the first 41 patients diagnosed with 2019-nCoV from Wuhan, China suggests that the virus acts similarly to SARS and MERS. Like the other two, 2019-nCoV causes pneumonia. But unlike those viruses, the new one rarely produces runny noses or intestinal symptoms, researchers report January 24 in the Lancet. Most of the people affected in that first group were healthy, with fewer than a third having chronic medical conditions that could make them more vulnerable to infection.
Disease tracker
An infection with a new coronavirus begins with an onset of symptoms including fever, cough and fatigue. Those symptoms can then intensify fairly quickly, resulting in hospital admission and acute respiratory disease syndrome, or ARDS (median time from onset of symptoms, shown).
How fast a new coronavirus can sicken


Where do new coronaviruses come from?
Coronaviruses are zoonotic, meaning they originate in animals and sometimes leap to humans. The first 2019-nCoV infections detected in December were in patients who had visited the Huanan seafood market in Wuhan. The market was closed January 1, but health officials have yet to determine from which type of animal the virus jumped to humans.
Bats are often thought of as a source of coronaviruses, but in most cases they don’t pass the virus directly on to humans. SARS probably first jumped from bats into raccoon dogs or palm civets before making the leap to humans. All the pieces necessary to re-create SARS are circulating among bats, though that virus has not been seen since 2004 (SN: 11/30/17).
MERS, meanwhile, went from bats to camels before leaping to humans (SN: 2/25/14). A paper published January 22 in the Journal of Medical Virology suggests that the new coronavirus has components from bat coronaviruses, but that snakes may have passed the virus to humans. But many virologists are skeptical that snakes are behind the outbreak (SN: 1/24/20).
How contagious are coronaviruses?
It depends on the coronavirus, but neither SARS or MERS have been able to sustain human-to-human transmission the way influenza viruses can, Fauci says. That’s because the viruses haven’t fully adapted to infect humans, “and maybe they never will,” he says.
Still, “this is a family of viruses that was formerly just the common cold,” he says. “But now, in the last 18 years, we’ve had three examples of it jumping species and causing serious disease in humans.” He and colleagues wrote an article published January 23 in JAMA to illustrate what they see as the growing threat from coronaviruses.
In Wuhan, the new coronavirus has been able to transmit down a chain of up to four people, health officials said. Five members of a family from Shenzhen, China caught the virus when they visited infected relatives in Wuhan, researchers report January 24 in the Lancet. Travelers have also carried the virus from China to at least seven other countries, including the United States. No human-to-human transmission has yet been reported outside of China, the WHO said. All of the deaths have also been in that country.
Epidemiologists are frantically calculating how infectious the new virus is, says Maimuna Majumder, a computational epidemiologist at Boston Children’s Hospital and Harvard Medical School.
The number that describes how many people a newly infected person is likely to pass a virus to is called R0, pronounced R naught (SN: 5/28/19). SARS, for instance, had an R0 between two and five, meaning that in a fully susceptible population an infected person could potentially spread the virus to two to five others. (Highly contagious measles, in comparison, has a R0 from 12 to 18.)
Estimates for the infectivity of the new virus range from the WHO’s estimate of 1.4 to 2.5 to a much bigger 3.6 to 4.0 calculation from Jonathan Read of Lancaster University in England and colleagues. Read’s group estimates that only about 5.1 percent of cases in Wuhan have been identified. The researchers reported the preliminary results January 24 at medRxiv.org.
That’s probably not because the Chinese government is covering up how bad the outbreak is, Majumder says. Many people may have had only mild symptoms or none at all. Those people probably wouldn’t go to the doctor and get tested for the virus.
Majumder and Harvard colleague Kenneth Mandl used a different method to calculate R0 for the new virus, estimating based on cases reported as of January 22 that its transmissibility falls from 2.0 to 3.3. Their results were posted to SSRN on January 23.
Meanwhile, Christian Althaus and Julien Riou, both of the University of Bern in Switzerland, posted data to Github supporting their calculation that the new virus’s infectivity is between 1.4 and 3.8. Each of those calculations was arrived at using different methods. While they are slightly different, they overlap, and Majumder says she’s reassured that the numbers are similar.
Similar infectivity to SARS doesn’t mean the new virus will spread like that one did.
“Having SARS in [our] history can help inform some these decisions that we’re going to make now. Back then, we were less prepared than we are now,” Majumder says.
What treatments are available?
For now, all doctors can do is treat symptoms of the new disease. Researchers have also developed some experimental treatments based on SARS and MERS, including antibodies that may help combat the infections, Fauci says.
Getting samples of the new virus may allow researchers to develop “monoclonal” antibodies in the lab. Or scientists may be able to take immune B cells from people who already have recovered from the virus to produce antibodies to help other infected people.
Some antiviral medications have shown promise in treating MERS, and are being tested for their effectiveness against 2019-nCoV. Experimental vaccines, Facui wrote in JAMA, including some based on RNA, are also in the works.
Erin Garcia de Jesus contributed to reporting of this story.







