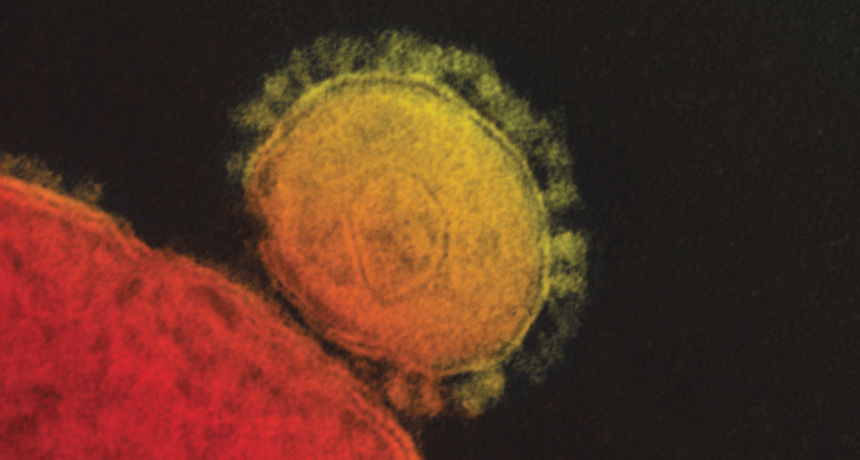
ACTIVE VIRUS A transmission electron micrograph shows the coronavirus responsible for Middle East respiratory syndrome in action.
NIAID
5
Outbreaks of two deadly viruses captured the world’s attention in 2013, but neither turned into the global pandemic expected to strike one of these years.
One of the viruses, known as MERS, causes Middle East respiratory syndrome.