Heal thy neighbor
Mental health services recruit locals to help residents of poor and war-torn countries
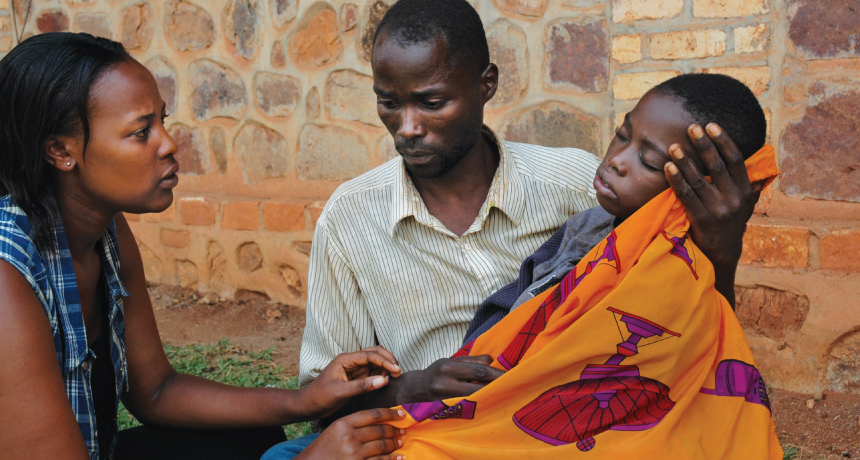
HOPEFUL HELP A psychosocial worker in Burundi in 2005 assists a boy with epilepsy and his father with mental health and epilepsy treatment.
Peter Ventevogel/HealthNet TPO
Nearly all the women of Mohmandara, a village in eastern Afghanistan near the Pakistan border, met at a local health clinic one day in 2005. Mental health workers at the clinic, run by a Dutch international aid organization, had heard village women talking to each other about “feelings of sadness” and “worrying too much.” The women eagerly accepted an invitation to talk it over at the clinic.
The village women described being beaten and harassed by their husbands, who were spurred on by their mothers and sisters. Families were imploding. Everyone in the group agreed that unemployment and poverty, in a land hounded by warfare, lay behind the surge of domestic violence.
With the help of a local woman trained by the aid organization, HealthNet TPO, the wives formulated a plan of action over several meetings. Close relatives were recruited to act as mediators between wives and their husbands’ families. The women practiced settling and defusing disputes at home. With help from another aid group, the wives raised money to buy chickens so they could sell eggs for added income.
Family life didn’t suddenly become tranquil. But for the first time, the village women felt hopeful that they could do something to reverse a deteriorating situation.
This emergency intervention was no isolated incident. Promising innovations in mental health care are popping up in some of the world’s most impoverished and devastated places. From Afghanistan to India, Uganda and beyond, a “take it to the people” model of psychotherapy is emerging. Stepping outside their traditional role as treatment providers, psychiatrists and psychologists train and supervise laypeople to deliver brief forms of group or individual psychotherapy. Early research suggests that inexpensive, nonprofessional therapists can effectively treat depression, anxiety and trauma-related problems, the most common mental ailments in the world today.
Scientists are beginning to explore the impact of war and lifelong hardships on mental health. One early discovery: Being accepted back into a family and community greatly alleviates suffering among former child soldiers, a fact that supports a growing international focus on social as well as psychological interventions.
“Humanitarian crises offer opportunities to build effective mental health care systems in developing nations,” says psychiatrist Vikram Patel of Sangath Centre, a nonprofit health organization in Goa, India. Massive emergencies focus attention and outside assistance on the psychological needs of survivors. Politicians presiding over distraught populations suddenly become receptive to redoing mental health systems.

In developing nations, where WHO estimates that there is an average of one psychiatrist serving anywhere from 200,000 to 1 million people, those who need mental health care usually don’t get it. Researchers say that a key to extending mental health care’s reach is to deploy available psychiatrists and psychologists as trainers and supervisors of nonprofessional counselors — including villagers in some of the world’s poorest and most violent regions. Lay counselors do the nitty-gritty work of coordinating each patient’s care, as well as providing brief group and individual psychotherapy to those who need and want it.
A 2013 WHO report titled “Building Back Better” describes how, in the aftermath of wars and natural disasters, ambitious mental health reforms have been instituted and are starting to make a difference in Afghanistan and 10 other countries and territories since 2000.
Many people living in war zones and impoverished communities suffer from a mix of mild to moderate depression, anxiety disorders and stress reactions to traumatic experiences, says Mark van Ommeren, a psychiatric epidemiologist at WHO in Geneva. Talk therapies adapted to specific cultures and lasting about six sessions show promise in easing these problems, he asserts. Psychiatric drugs can be used if needed with brief psychotherapy.
“There is an enormous need for mental health services, and it can’t be met without training generalists who treat people in their own communities,” van Ommeren says.
No humiliating labels
One of the most ambitious efforts to build and study a mental health care system that puts nonprofessionals on the front lines is happening in Goa, a small state on India’s west coast. This project, directed by Patel, encourages everyone from health counselors to psychiatrists to refer to patients’ emotional problems with local terms, not psychiatric labels viewed as humiliating and shameful in Indian cultures. “We never say ‘depression’ or ‘mental illness’ when treating patients,” Patel explains. “That vocabulary isn’t culturally appropriate.”
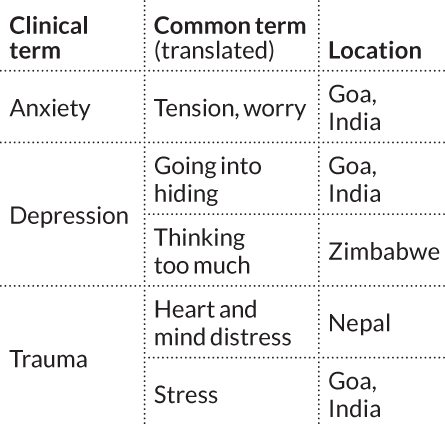
Patients in Goa often speak of anxiety problems as “tension” or “worry,” and describe depression as “going into hiding.” Health counselors use those terms to inquire further about a person’s daily problems and to develop a treatment plan.
Patel led an investigation called MANAS that evaluated how effectively nonprofessionals treated poor and working-class people with common mental disorders. MANAS is an acronym for “project to promote mental health” in India’s Konkani language. Treatment trials ran from April 2007 to September 2009 at 12 public primary health care centers and in 12 private medical practices.
Researchers tracked nearly 2,800 adult patients with depression and other common mental ailments, most for one year. Roughly half of these individuals received care coordinated by locally recruited health counselors who completed two months of training organized by MANAS researchers.
Health counselors provided information about symptoms and treatment, referrals to social welfare agencies, advice about breathing exercises and other strategies to lessen anxiety, and six to 12 sessions of interpersonal psychotherapy adapted for India. Developed in the United States, interpersonal psychotherapy addresses ways to strengthen relationships and counteract triggers of depression in a person’s life.
Primary care physicians prescribed medications for depression or anxiety to about one-third of psychotherapy patients, in consultation with a psychiatrist who also treated especially troubled individuals referred by health counselors.
Another group of patients in the trials received mental health care from primary care physicians who could consult treatment manuals prepared by the MANAS team.
Interpersonal psychotherapy and other interventions delivered by health counselors substantially relieved patients’ depression and improved their work and home lives for up to one year after treatment started, Patel and his colleagues report in the April British Journal of Psychiatry. Physician-led care produced more modest benefits.
In Uganda and Brazil, Patel’s group notes, recent trials produced similar gains for depressed patients who received brief psychotherapy and other services from trained nonprofessionals.
Even with the cost of training and hiring health counselors for MANAS, mental health treatment cost less when led by nonprofessionals than by physicians, at least in public facilities, Patel and other researchers reported in a 2012 Bulletin of the World Health Organization.
Efforts are underway to expand MANAS throughout India.
Group relief
In a rural part of the Democratic Republic of the Congo that has been plagued by warfare for nearly 20 years, women have had no access to professional help to deal with the emotional aftereffects of rape and other conflict-related ordeals. Clinicians and researchers are beginning to bring brief psychotherapy to these beleaguered people and others like them who live far from cities, hospitals or safe havens.
Group psychotherapy delivered by trained nonprofessionals shows particular promise in such settings.
Psychiatric epidemiologist Judith Bass of Johns Hopkins University led a project that successfully treated trauma-related problems among Congolese women (SN Online: 6/6/13). Bass’ team trained Congolese women who had experience in assisting rape survivors to provide either group therapy or individual support to 405 traumatized women in 15 villages. Most of those getting help had been raped by government or rebel soldiers.
Groups of six to eight women received up to 12 sessions of cognitive processing therapy, a treatment for post-traumatic stress disorder developed in the United States more than 20 years ago. Lay counselors, supervised weekly by a Congolese social worker trained in the therapy, focused on getting rape survivors to stop blaming themselves for their misfortune and to formulate strategies for moving on with their lives. Women receiving individual support mainly received medical and social welfare referrals.
Six months after treatment, the proportion of women with probable PTSD had dropped from 60 percent to 9 percent in the cognitive processing therapy group, with similar declines for depression and anxiety. About half of the women who had received individual support still struggled with PTSD symptoms, depression and anxiety six months later.
“We saw women who once felt stigmatized reengage with their families and communities after receiving cognitive processing therapy,” Bass says.
Evidence of group therapy’s benefit comes from northern Uganda as well, where civil war raged from 1987 to 2008. Men and women who attended two to five monthly group counseling sessions displayed faster reductions in PTSD symptoms and depression over the next three months than individuals who declined counseling sessions. Group meetings helped participants — including 10 individuals infected with HIV — function better at work and at home, psychiatrist Etheldreda Nakimuli-Mpungu of Makerere University in Kampala, Uganda, and her colleagues reported in the October Journal of Affective Disorders.
In that study, counselors and social workers at four privately funded trauma clinics in northern Uganda conducted group sessions with 69 volunteers already receiving antidepressants or other medications for mental ailments. Ugandans participating in those groups shared trauma stories, learned relaxation techniques and devised new ways to cope with their lives.
Impacts of poverty vs. war
In developing countries, war isn’t the only threat to mental health. One long-term investigation indicates that extreme poverty and social discrimination inflict a brand of emotional harm apart from that caused by living through violent conflicts.
In the South Asian nation of Nepal, many people have endured episodes of depression set off not by wartime experiences but by lifelong poverty and social mistreatment, says Brandon Kohrt, a medical anthropologist and psychiatrist at Duke University School of Medicine. In contrast, among poor Nepalese villagers, violent experiences during a prolonged civil war — but not economic hardships and other stresses unrelated to the war — triggered anxiety problems, including intrusive memories of life-threatening events and other cardinal signs of PTSD, Kohrt and his colleagues reported in the October 2012 British Journal of Psychiatry.
“War has been assumed to increase rates of depression and anxiety alike, but that wasn’t the case when we tracked mental health before and after Nepal’s conflict,” Kohrt says.
Cognitive behavioral therapy and a few other types of brief psychotherapy work well at easing mild to moderate depression and anxiety in Western nations. Kohrt studied whether culturally customized versions of these treatments could do the same in countries where depression and destitution go hand in hand.
He and his colleagues asked nearly 300 Nepalese villagers to complete assessments of depression and anxiety in 2000, about a year before a war began between government and rebel forces. Villagers responded to the same surveys again in 2007, about a year after violence ended.
The proportion of depressed villagers rose from 31 percent to 41 percent, a trend largely explained by the aging of this population, Kohrt says. Depression most frequently affected the poorest villagers, who belonged to one of Nepal’s lowest social castes. His team estimates that being in a low caste — and thus facing perpetual social exile by neighbors from higher castes — inflamed depression among Nepalese villagers as much as the most severe war traumas triggered PTSD and other anxiety disorders.
Anxiety ailments increased from 26 percent to 48 percent, a trend that exceeded what could be attributed to aging. Villagers who had witnessed armed groups murder people and experienced other wartime ordeals reported the worst anxiety symptoms. About 14 percent had PTSD.
Some clinicians say that non-Western victims of life-threatening events don’t react in ways that neatly fit within U.S. psychiatry’s official definition of PTSD. Western psychiatrists focus on individuals’ reactions to specific traumas, such as being raped or witnessing a comrade’s death during combat. In family- and community-oriented countries emerging from years of civil war, many people are traumatized by the loss of traditional social ties and rampant mistrust among survivors, including relatives, some researchers contend. Community-wide programs that repair the social fabric may have more potential in these settings than individual or group psychotherapy.
Open arms
The power of social forces to mend or aggravate war’s emotional wounds resonates loudly among former child soldiers. Tens of thousands of children under age 18 currently serve in government forces or armed opposition groups.

Her team studied 243 former child soldiers, most in their late teens, in the African nation of Sierra Leone. These young people typically got abducted into a rebel army during childhood and spent several years with their captors acting as spies, porters, fighters and — mainly among 73 girls in the sample — sex slaves.
From 2004 to 2008, PTSD rates declined from 32 percent to 16 percent, although few youngsters received formal counseling of any kind, Betancourt’s group reports in the September British Journal of Psychiatry.
Stress symptoms cleared up the most among ex-soldiers who were openly welcomed back into their families and communities. Those who returned home only to experience a parent’s death or threats and abuse from community members tended to get worse.
Former child soldiers who faced rejection in their communities also reported escalating loneliness, depression, anxiety, stealing and fighting, the researchers report September 14 in the Journal of Child Psychology and Psychiatry.
Kohrt has reported similar findings for former child soldiers in Nepal. His team worked with private aid groups and residents of several villages to find ways to support returning youngsters. Strategies included holding public welcome-back ceremonies and encouraging ex-soldiers to return to school and join sports or drama clubs.
Effective treatments, Kohrt says, need to follow the lead of India’s MANAS program and employ language that defuses cultural stigmas about mental ailments.
“With former child soldiers in Nepal, we used ‘heart and mind distress’ as a general term for bad memories and other trauma symptoms,” he says. “That made it easier for them to talk.”
Like soldiers anywhere, Kohrt adds, ex-child combatants in Nepal who suffered the worst emotional problems experienced a “double hit” of trauma. Youngsters first got steamrolled by the awfulness of war. Then they were blindsided by rejection and mistreatment upon returning home.
In Nepal, girls who had been abducted into rebel groups suffered the harshest double hit. These kids had been forced to be sex slaves, yet their defilement marked them as unacceptable to families and communities. Girls, far more than boys, suffered from lasting PTSD, Kohrt says. He and his colleagues plan to work with aid organizations to help incorporate these girls back into schools and social clubs.
A hard road
Kohrt knows that it’s an uphill battle to treat the mental aftereffects of long-term conflicts. But opportunities for revamping psychological care continue to sprout from the rubble of social and natural disasters.
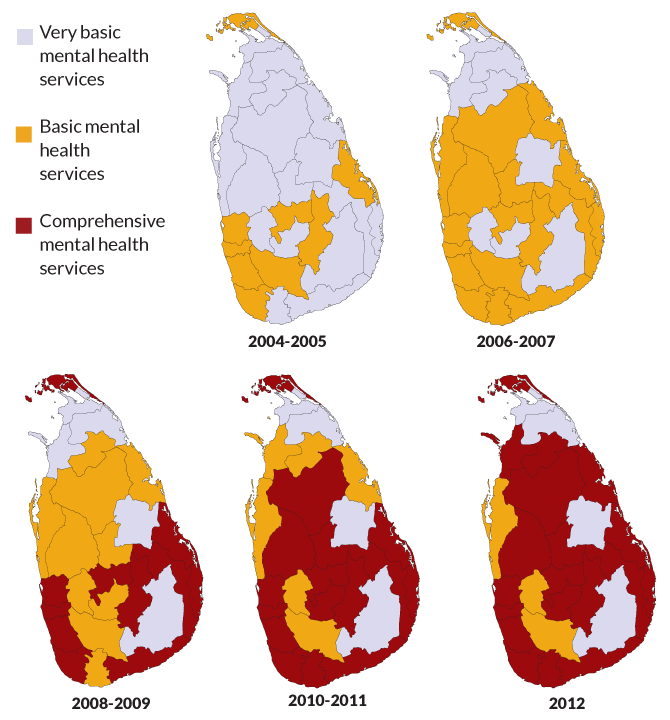
Consider Sri Lanka, a teardrop-shaped island off India’s southern coast. The new WHO report outlines how, following a devastating 2004 tsunami, this nation parlayed international aid into a network of community mental health services that collaborate with hospitals and outreach clinics.As in Afghanistan, locally recruited lay mental health workers in Sri Lanka build trust with families and refer people in need to outreach clinics that have been established in many parts of the country.
Although the tsunami attracted worldwide publicity, Sri Lankans also struggle with the emotional repercussions of a less well-known civil war. More than 100,000 Sri Lankans were killed and many more injured or displaced between 1983 and 2009, according to a report in the January International Journal of Mental Health Systems. To deal with both tragedies, Sri Lanka’s mental health system needs to go beyond psychotherapy and experiment with community interventions, including organizing public mourning and healing ceremonies and forming women’s groups and youth clubs, say psychiatrists Daya Somasundaram of the University of Jaffna in Sri Lanka and Sambasivamoorthy Sivayokan of the University of Adelaide in Australia.
In Libya, the emotional wounds of war are fresher. Heavy fighting in Libya throughout 2011 resulted in an urgent need for mental health care, remarks WHO’s van Ommeren. “WHO is now active in a program to build a new, community-based mental health system in Libya,” he says.
That effort, coordinated by WHO and Libya’s Ministry of Health, is training the nation’s small number of psychologists in brief psychotherapy for ex-combatants and their families. Lay counselors will be trained to identify common mental ailments and refer people for psychological care.
Poverty, oppression and warfare will continue to generate a need for neighbor-based therapy and community-strengthening interventions in many parts of the world. Lessons learned in today’s zones of conflict and deprivation will likely influence mental health care for years to come.
Tough times for U.S. psychotherapy
Talk therapy is declining in the land of the free and the home of the medicated. Epidemiologist Myrna Weissman of Columbia University sees a bitter irony in that trend.
“Psychotherapy is becoming less accessible in the United States as it is being enthusiastically embraced in developing countries hurt by HIV, natural disasters, wars or political strife,” says Weissman, codeveloper of a brief form of psychotherapy called interpersonal therapy.
From 1998 to 2007, the proportion of patients in U.S. outpatient mental health clinics receiving psychotherapy alone fell from 15.9 percent to 10.5 percent, while the proportion prescribed medication alone rose from 44.1 percent to 57.4 percent. Primary care physicians, who treat most cases of depression and other common mental ailments, increasingly prescribe psychoactive medications as well.
Yet a growing number of studies show that interpersonal therapy, cognitive behavioral therapy and a few other talk therapies — most lasting 20 sessions or fewer — help patients and their families more over the long run than medication does, with far fewer side effects. Surveys consistently find that depressed patients and their families would prefer psychotherapy over medication.
In an editorial in the Sept. 29 New York Times, psychologist Brandon Gaudiano of Alpert Medical School of Brown University argued that professional psychotherapy organizations must launch aggressive educational campaigns to burnish talk therapy’s tarnished image.
Real progress in reducing mental disorders will require dramatic changes in how interventions are delivered, Gaudiano and Brown University psychologist Ivan Miller wrote in the November Clinical Psychology Review. That shift in distribution includes forming mental health care teams with psychotherapists supervising physicians and lay counselors. Efforts to do just that are under way in the United Kingdom and several other Western nations, but not in the United States, says psychiatric epidemiologist Mark van Ommeren of WHO in Geneva.
A network of inexpensive, community-based lay counselors trained in one or more brief psychotherapies, able to refer severe cases to professionals, would be a big step forward for U.S. mental health care, says psychiatrist Vikram Patel of Sangath Centre in Goa, India. In this setup, psychotherapy would be provided in schools, community centers and homes, not hospitals and offices.
“Western mental health professionals need to appreciate that, for most people, their mental health and their daily lives are integrally connected,” Patel says. “It’s not like having a boil on your back.” — Bruce Bower