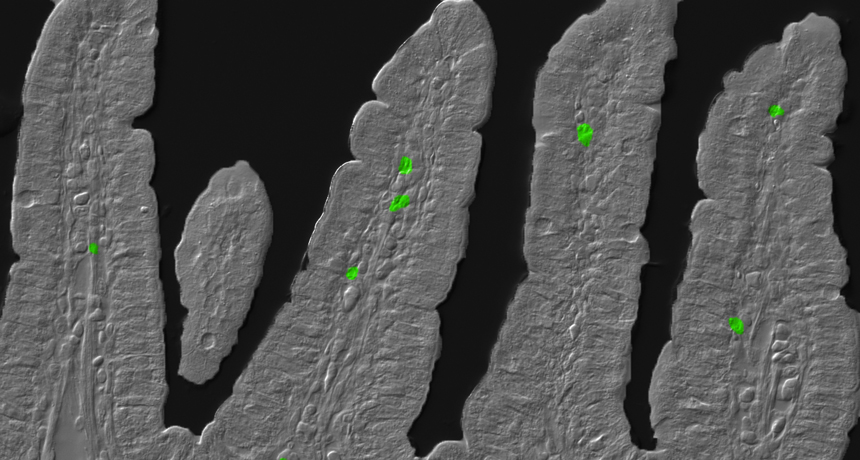
UPSET CLOCK Disrupting a mouse’s internal clock boosts the abundance of one type of immune cell, TH17 (false-colored green), in the lining of the intestines (gray fingerlike projections). The extra immune cells may make animals prone to inflammatory diseases.
Courtesy of Xiaofei Yu, Shipra Vaishnava and Yuhao Wang